What is Bruxism?
Smile Perfected & most dental professionals would say teeth grinding, and they would be mostly correct.
However, there is no widely accepted definition of bruxism4, but some suggested definitions include:
- “A movement disorder of the masticatory system characterized by teeth grinding and clenching during sleep as well as wakefulness.”1
- “Periodic repetitive clenching or rhythmic forceful grinding of the teeth.”2
- “Parafunctional grinding of teeth or an oral habit consisting of involuntary rhythmic or spasmodic non-functional gnashing, grinding or clenching of teeth in other than chewing movements of the mandible which may lead to occlusal trauma.”3
- “Non-functional contact of the mandibular and maxillary teeth resulting in clenching or teeth grinding due to repetitive, unconscious contraction of the masseter and temporalis muscles.”5
- The ICSD-R described three different severities of sleep bruxism, defining mild as occurring less than nightly, with no damage to teeth or psychosocial impairment; moderate as occurring nightly, with mild impairment of psychosocial functioning; and severe as occurring nightly, and with damage to the teeth, temporomandibular disorders and other physical injuries, and severe psychosocial impairment.6
- The Individual (personal) Tooth-Wear Index was developed to objectively quantify the degree of tooth wear in an individual without being affected by the number of missing teeth.3
Properly Diagnosing Bruxism
The wide range of classifications and definitions can leave dental practitioners searching for answers.
The diagnosis of bruxism is where dentists should focus.
Patients should be diagnosed in three different stages of bruxism: Mild, Moderate & Severe.
Once bruxism severity is determined, the proper thickness of a custom grind guard can be made for the patient.
The illustration below is a reference tool for determining the type of bruxism.
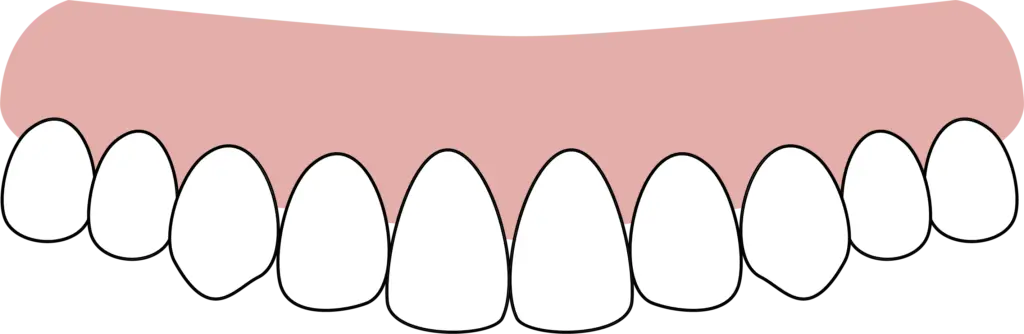

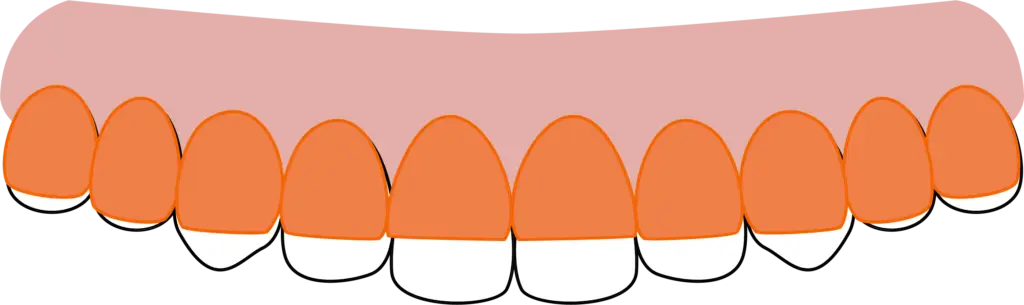
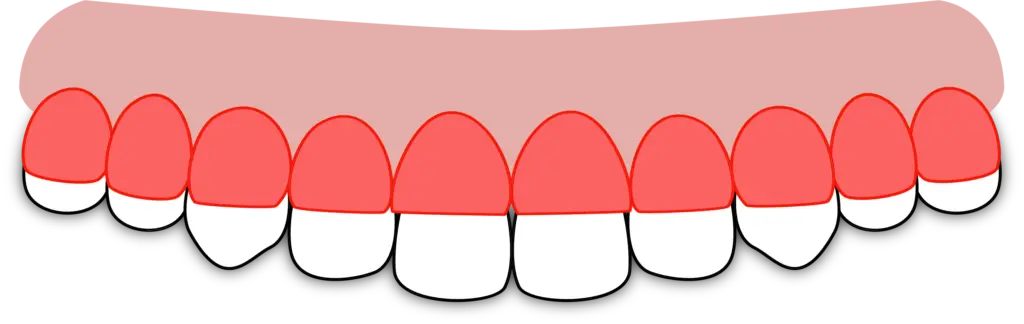
Assessing the amount of enamel and dentin that has been ground away is the best tool.
Understanding each level of teeth grinding in detail is key for proper treatment during any bruxism stage.
Class I: Mild Bruxism

Clinical signs and symptoms of Mild Bruxism include a patient stating that they know or have been told they grind or clench their teeth.
They are normally told this is the early stages of grinding teeth by their significant other or a dental professional.
Grinding or clenching noises, typically at night, verify this.
Upon clinical examination of the patient, they would show signs or symptoms of one or more clinical findings:
- Masseteric hypertrophy (Enlargement of jaw muscle)
- Trismus (Locking of the jaw)
- Cheek & Lip biting,
- Burning sensation of the tongue
- Headaches
- Migraines
- Indentations on the tongue along the occlusal plane
- Hypersensitive teeth
- Pain in the muscles of mastication
- Tenderness of the TMJ to palpation
- Clicking or locking of the temporomandibular joints.

In addition to any of the bruxism symptoms listed above, there would be minor tooth attrition of less than 1mm of enamel wear on the cusp tips or incisal edges of teeth not due to normal tooth wear.
In cases of mild grinding diagnosis, a lighter hard-soft grinding appliance between 1.5 MM and 3 MM in thickness is recommended.
Class II: Moderate Bruxism

In addition to any signs and symptoms listed above, there would be moderate tooth attrition with 1-2mm of enamel loss but no dentin exposed on the cusp tips or incisal edges of the teeth not due to normal tooth wear.
A lighter hard-soft grinding appliance is recommended between 2 MM and 4 MM in thickness in cases of moderate grinding diagnosis.
Class III: Severe/Advanced Bruxism

In addition to any of the signs and symptoms listed above, there would be extreme tooth attrition with greater than 2mm of enamel loss with dentin exposed on the cusp tips or incisal edges not due to normal tooth wear.
These are clear indicators of the suffering patients are dealing with when it comes to severe bruxism.
A lighter hard-soft grinding appliance is recommended between 3 MM and 5 MM in thickness in cases of severe grinding diagnosis.
100% Acrylic appliances, 3 MM – 6 MM thick, are also recommended, but patient compliance is lower due to uncomfortable fit.
Hard-soft night guards may wear down more rapidly. However, these are recommended since patient compliance is higher because of the more comfortable fit.
It should be noted that the presence of tooth wear only indicates that it has occurred at some point in the past, and does not necessarily indicate that the loss of tooth substance is ongoing.
The loss of tooth substance can be severe in some cases.
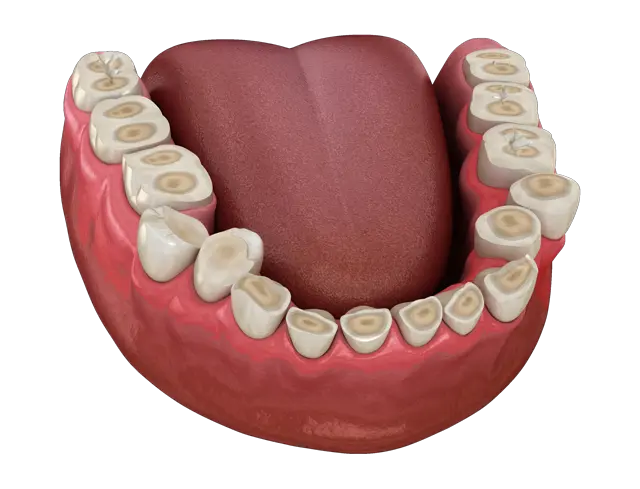
The exposure of dentin, secondary dentin, and pulp is a direct cause of even minor untreated bruxism over time. This exposure can lead to major dental reconstructive work.
Protecting the teeth before this situation is recommended.
Patients frequently resist the doctor’s recommendation since grind guards can be expensive and uncomfortable.
The dentist should explain to the patient the long-term pain and expense of crowns and implants.
Dental practices can use their 3D scanner to show the patient the damage being done by grinding.
Informing the Patient as a Dentist
All dentists see it…patients who grind and clench their teeth.
As dentists, we see it, and we pause. UGH!!
We ask the question to ourselves:
“As a dentist, what do I do about this patient’s teeth grinding?”.
Do I tell the patient? If I tell the patient about their grinding, then the patient may want a solution to stop the grinding.
It is important to let the patient know we can’t stop grinding. The patient is slowly destroying their teeth and their smile.
However, we want to help stop the grinding and clenching.
An occlusal/night guard is the best solution to this problem.
The treatment strategy to use is protection and tooth loss prevention. Dental professionals must help the patient avoid further damage to their teeth and smile.
As a dentist, you are responsible for telling the patient they are grinding. This should be documented in the patient’s chart.
The recommendation for an occlusal/night guard should also be noted.
It is not typical for a dentist to be able to get a patient to stop grinding or clenching.
Grinding and clenching are so multi-factorial that a dentist is not trained in all the fields of medicine and psychiatry to “fix” the problem of grinding and clenching.
Bruxism is commonly associated with stress, but there are many other factors.
A custom-fit occlusal/night guard is the best solution to this problem.
Want to learn more about adding bruxism diagnosis to your dental practice?
Check out our FREE online dental practice management course hosted by Dr. William L Balanoff.

Article Resources
- Wassell R, Naru A, Steele J, Nohl F (2008). Applied occlusion. London: Quintessence. pp. 26–30.
- Cawson RA, Odell EW, Porter S. (2002). Cawsonś essentials of oral pathology and oral medicine. (7th ed.). Edinburgh: Churchill Livingstone. pp. 65,66,364,366.
- Shetty, S; Pitti, V; Satish Babu, CL; Surendra Kumar, GP; Deepthi, BC (2010 Sep). “Bruxism: a literature review.”. Journal of Indian Prosthodontic Society 10 (3): 141–8.
- Lobbezoo, F.; van der Zaag, J.; Naeije, M. (1 April 2006). “Bruxism: its multiple causes and its effects on dental implants – an updated review*”. Journal of Oral Rehabilitation 33 (4): 293–300.
- Persaud, R; Garas, G; Silva, S; Stamatoglou, C; Chatrath, P; Patel, K (2013 Feb). “An evidence-based review of botulinum toxin (Botox) applications in non-cosmetic head and neck conditions.”. JRSM short reports 4 (2): 10.
- “International classification of sleep disorders, revised: Diagnostic and coding manual.”. Chicago, Illinois: American Academy of Sleep Medicine, 2001. Retrieved 16 May 2013.

